Research in Focus: Path-Breaking Work from Michigan Public Health

Apple Study: Noise-Induced Hearing Loss and Your Health
 University of Michigan researcher Rick Neitzel has teamed up with Apple for a groundbreaking
new study that examines sound exposure and its impact on hearing health.
University of Michigan researcher Rick Neitzel has teamed up with Apple for a groundbreaking
new study that examines sound exposure and its impact on hearing health.
The Apple Hearing Study is one of three new studies now available on Apple’s Research app that explore new areas of medical research.
“The study will measure user levels of sound exposure and determine how these exposures impact hearing and stress levels,” said Neitzel, an associate professor of Environmental Health Sciences and Global Public Health at the University of Michigan School of Public Health, who will lead the work.
The analysis of this data over time will give researchers a better understanding of listening behavior, and how everyday sound exposure can impact hearing and overall human health. “This unique dataset will allow us to create something the US has never had—national-level estimates of exposures to music and environmental sound,” Neitzel said.
Many Americans think of noise as just an occupational hazard—and as an industrial hygienist, that’s been my focus historically. But most of us fail to realize that we can get a lot of noise elsewhere in our lives.
—Rick Neitzel, Associate Professor of Environmental Health Sciences
“Collectively, this information will help give us a clearer picture of hearing health in America and will increase our knowledge about the impacts of our daily exposures to music and noise. We’ve never had a good tool to measure these exposures. It’s largely been guesswork, so to take that guesswork out of the equation is a huge step forward.”
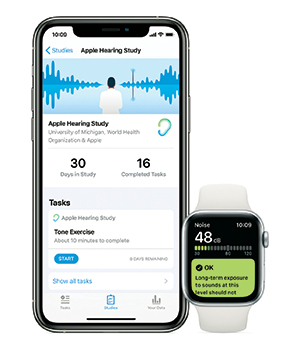 How sound exposure impacts hearing health has not been well understood because researchers
lack the tools to measure daily sound exposure over time. Researchers hope to use
the capabilities and ubiquity of Apple products to conduct this large-scale study.
How sound exposure impacts hearing health has not been well understood because researchers
lack the tools to measure daily sound exposure over time. Researchers hope to use
the capabilities and ubiquity of Apple products to conduct this large-scale study.
“Noise exposure is an emerging challenge that carries serious health implications for people worldwide,” said Rebecca Cunningham, University of Michigan vice president for research. “The University of Michigan certainly cannot address this public health threat alone, which is why our partnership with Apple is so critical.
“These types of industry partnerships play a vital role in the overall health of our research enterprise, and by working together, researchers and industry leaders can help solve important issues facing our society,” Cunningham said.
Why is noise-induced hearing loss important?
 Noise is a common environmental sound exposure around the world. The most well-understood health impact of noise—noise-induced hearing loss (NIHL)—is
also one of the most common illnesses globally. Individuals afflicted with NIHL suffer
from a wide variety of adverse social, health, and occupational impacts. These can
include communication and relationship difficulties; social withdrawal and isolation;
reduced quality of life; depression and mental health issues; and, potentially, loss
of employment. Additionally, children and young adults suffering from NIHL have substantial
lifelong educational-related impacts. While often considered more of a nuisance than
a disease, NIHL is in fact a debilitating—but entirely preventable—condition.
Noise is a common environmental sound exposure around the world. The most well-understood health impact of noise—noise-induced hearing loss (NIHL)—is
also one of the most common illnesses globally. Individuals afflicted with NIHL suffer
from a wide variety of adverse social, health, and occupational impacts. These can
include communication and relationship difficulties; social withdrawal and isolation;
reduced quality of life; depression and mental health issues; and, potentially, loss
of employment. Additionally, children and young adults suffering from NIHL have substantial
lifelong educational-related impacts. While often considered more of a nuisance than
a disease, NIHL is in fact a debilitating—but entirely preventable—condition.
How is noise-induced hearing loss measured?
 NIHL can be assessed in several ways. Our study utilizes two different tests: pure tone audiometry and speech-in-noise.
Pure tone audiometry measures how much sound it takes a person to hear at different
frequencies. Participants are presented with a pure tone stimulus at a range of different
frequencies, and their hearing ability at each frequency is measured in decibels of
hearing level. The speech-in-noise test measures how well a person hears words in
the presence of background noise. This test provides a measure of functional word
recognition in background noise, and is summarized as a speech recognition threshold.
NIHL can be assessed in several ways. Our study utilizes two different tests: pure tone audiometry and speech-in-noise.
Pure tone audiometry measures how much sound it takes a person to hear at different
frequencies. Participants are presented with a pure tone stimulus at a range of different
frequencies, and their hearing ability at each frequency is measured in decibels of
hearing level. The speech-in-noise test measures how well a person hears words in
the presence of background noise. This test provides a measure of functional word
recognition in background noise, and is summarized as a speech recognition threshold.
—Rick Neitzel
Lead image above. Data from Neitzel’s work is being shared with the World Health Organization’s “Make Listening Safe” initiative to inform new policies around hearing health around the world.
For Children, Food Insecurity Means Not Only Hunger but Stress, Sadness
A new study led by University of Michigan School of Public Health researchers shows that children know more about food insecurity—the state of being without reliable access to a sufficient quantity of affordable, nutritious food—than their parents give them credit for.
Our research shows that children are not only aware that their family is food insecure but are also psychologically impacted by it.
—Cindy Leung, Assistant Professor of Nutritional Sciences
 “The long-held assumption is that parents will do whatever it takes to protect their
children from food insecurity,” said Cindy Leung, assistant professor of Nutritional
Sciences and lead researcher in the study. “Our research shows that children are not
only aware that their family is food insecure but are also psychologically impacted
by it.”
“The long-held assumption is that parents will do whatever it takes to protect their
children from food insecurity,” said Cindy Leung, assistant professor of Nutritional
Sciences and lead researcher in the study. “Our research shows that children are not
only aware that their family is food insecure but are also psychologically impacted
by it.”
Researchers talked to 60 children from the San Francisco Bay area. The children discussed worrying about not having enough food and about their parents’ well-being, embarrassment about the family’s situation, strain on family dynamics due to food insecurity, and sadness over not having enough food.
“We think of food insecurity as just a food problem, so our interventions are to provide food,” Leung said. “But food is more than just calories. When you don’t have enough, it impacts your physical health and your mental well-being, and our interventions to address food insecurity should focus beyond just the provision of food.”Full Influenza Vaccination among Children Cuts Hospitalization in Half
 Fully vaccinating children reduces the risk of hospitalization associated with influenza
by 54 percent, according to a study by researchers at the University of Michigan School
of Public Health, the Clalit Research Institute, and Ben-Gurion University in Israel.
The study is one of the few worldwide that has tested the effectiveness of childhood
vaccination against influenza and risk of hospitalization due to influenza complications.
In Israel, as in the US, government guidelines recommend that children eight or younger
who have never been vaccinated, or who have only gotten one dose of flu vaccine previously,
should receive two doses of vaccine.
Fully vaccinating children reduces the risk of hospitalization associated with influenza
by 54 percent, according to a study by researchers at the University of Michigan School
of Public Health, the Clalit Research Institute, and Ben-Gurion University in Israel.
The study is one of the few worldwide that has tested the effectiveness of childhood
vaccination against influenza and risk of hospitalization due to influenza complications.
In Israel, as in the US, government guidelines recommend that children eight or younger
who have never been vaccinated, or who have only gotten one dose of flu vaccine previously,
should receive two doses of vaccine.
Study Links Common Chemicals to Preterm Births in Puerto Rico
Seeking answers to what is behind high rates of preterm birth in Puerto Rico, researchers have found an association between exposure to chemicals commonly found in many consumer products and a shorter duration of pregnancy and increased risk of preterm birth. John Meeker, professor of Environmental Health Sciences at the School of Public Health, and colleagues from several US research universities found that higher urinary concentrations of phthalate metabolites in women translated to 42 percent greater odds of having preterm births—before 37 weeks—compared with women with lower exposures.
“Women with exposure levels bordering the highest 25 percent of the population, on average, had a pregnancy that was one-and-a-half days shorter than women whose exposure was bordering the lowest 25 percent,” Meeker said.
Phthalates are found in personal care products, such as perfumes, deodorants, and lotions, and in food, adhesives, vinyl flooring, plastic shower curtains, and some medications. Preterm birth is a global concern, and Puerto Rico not only has one of the highest rates in the US but is among the highest in the world. “Our findings suggest certain phthalates may play a role in the risk of having a preterm birth in Puerto Rico and elsewhere, but there are likely other risk factors as well,” Meeker said.New Research Reviews Opioid Misuse Prevention Policies across US
In an effort to combat the opioid crisis, states are implementing an array of preventive measures to address the health consequences of opioid misuse and addiction. In recently published research, School of Public Health PhD students Amanda Mauri and Tarlise Townsend aggregated the various types of interventions into a single paper and review of findings.
“Our review informs decision-making around which opioid misuse prevention policies public officials should implement,” said Mauri, PhD student in the Department of Health Management and Policy and first author on the paper. “Specifically, public officials can use our findings to determine which policies will likely be most effective at addressing opioid prescribing and overprescribing.”
The research suggests that drug supply management policies, such as policies requiring prior authorization for specific opioids or dosages, reduced overall opioid prescribing and dosage prescribed. Robust prescription drug monitoring programs were also found to reduce prescribing. In addition to looking at policies for which evidence is already available, the review also highlights areas where future research should concentrate. “The majority of the included articles assessed prescription drug monitoring programs. We recommend that researchers consider focusing on other interventions that have not received sufficient evaluation, such as Good Samaritan Laws and naloxone access laws,” Mauri said. Another opportunity for researchers to explore are unintended consequences of opioid misuse prevention policies and differential policy effects across populations.Screening for Lung Cancer Based on Risk Could Save Lives
 Changing the way individuals are selected to be screened for lung cancer, by considering
their probability of getting or dying from lung cancer calculated from risk-prediction
models, could prevent 14 percent of lung cancer deaths per year, according to a new
study.
Changing the way individuals are selected to be screened for lung cancer, by considering
their probability of getting or dying from lung cancer calculated from risk-prediction
models, could prevent 14 percent of lung cancer deaths per year, according to a new
study.
The Cancer Intervention and Surveillance Modeling Network (CISNET) Lung Working Group, which includes researchers from the School of Public Health, says this means nearly 2,000 deaths could be prevented annually in the US by factoring more information from the many risk-prediction models developed in recent years that consider a person’s risk factor profile.
“The results of this study are of major importance for the implementation of lung cancer screening worldwide,” said Rafael Meza, associate chair of Epidemiology at the School of Public Health and coordinating principal investigator of the CISNET lung group. “Risk-based screening strategies have the potential of saving more lives.”- Interested in public health? Learn more today.
- Read more articles by researchers at Michigan Public Health.
- Support research at Michigan Public Health.
Tags
- Faculty
- Spring 2020
- Staff
- Students
- Adolescent Health
- Cancer
- Child Health
- Chronic Disease
- Environmental Health
- Epidemiology
- Food Safety
- Health Care Management
- Health Communication
- Health Informatics
- Infectious Disease
- Innovation
- Mental Health
- Nutrition
- Opioids
- Pregnancy
- Reproductive Health
- Research
- Toxicology
- Vaccines
