Safe Labor, Industry, and Business during a Pandemic

Q&A with Aurora Le
Assistant Professor of Environmental Health Sciences
As states in the US slowly reopen their economies, industry and business leaders will need to evolve how they think about worker safety to include a range of measures related to mitigating the spread of infectious disease.
We recently connected with Aurora Le, assistant professor of Environmental Health Sciences at the University of Michigan School of Public Health. Le's research areas include highly infectious diseases and occupational safety and health. She works with the Biosafety and Infectious Disease Training Initiative (BIDTI) and supported the research efforts of the Nebraska Biocontainment Unit after the treatment of three Ebola patients there in 2014–2015.
Le has been working closely with other public health researchers to understand how occupational health practices can help protect us from exposure to the coronavirus as we return to work. As our industries and services begin to reopen, we asked her about high- and low-risk settings and how managers, owners, and industry leaders can be thinking about workplace safety during a pandemic.
There are thousands of different workplaces in Michigan alone. How do public health experts arrive at designations of high, medium, and low risk for different industry sectors and different types of jobs?
We start by asking what aspects of each job type—specific to industry—might put workers at risk of exposure to the virus. The current team of occupational health and epidemiology experts at Michigan Public Health working on workplace pandemic response distilled the process down to eight factors we think determine what risk of exposure might be:
- Do you interact with the general public?
- Do you have close interactions or direct physical contact with your coworkers?
- Are you sharing tools or machinery or office equipment?
- Are you having to travel to many different sites over the course of your job?
- Do you work in an area where there's a high density of workers, in other words, each worker doesn't have very much space basically to themselves?
- Are you working indoors or outdoors?
- Are you working in a building that has pretty good ventilation or outside, or are you trapped in a space that doesn't have much air movement?
- And finally, how much access do you have to sanitation facilities, hand washing stations, or hand sanitizer stations?
These eight factors help us determine which industries, job types, workplaces, and workstations create a high, medium, or low risk of infection for workers. Once you understand your risk level, the goal is for any high- or medium-risk location to move itself to a position of lower risk by implementing new safety measures and/or improving the processes and measures they already have in place.
What are some specific changes we might see in a high-risk industry or workplace?
A good example of a high-risk group is someone working in outpatient health care services—where patients visit for provider office visits and nonurgent medical procedures. Virtual visits via phone calls or video chats will continue to be encouraged if there is not an urgent need to be seen in-person. Something like a rash or minor bump could be shown to a provider on a video chat, and if a prescription is needed, it can be sent to a local or mail-order pharmacy.
We can expect to see barriers or shields at check-in, fewer seats in waiting areas, and even separate waiting areas for people experiencing high temperatures. You might also see virtual check-in prior to an in-person visit, where you wait in the car until you are called in for the appointment. We will see more signage about infection control, strong encouragement for patients to wear a provided mask or come in wearing their own mask, and more hand sanitizing stations. Health care workers will be undergoing self-check measures like daily temperature checks and symptom diaries before beginning the work day.
What might things look like in a restaurant?
Restaurants actually have some experience with infectious disease control from a food safety perspective, since food service locations can “seed” outbreaks of things like e. Coli or hepatitis.
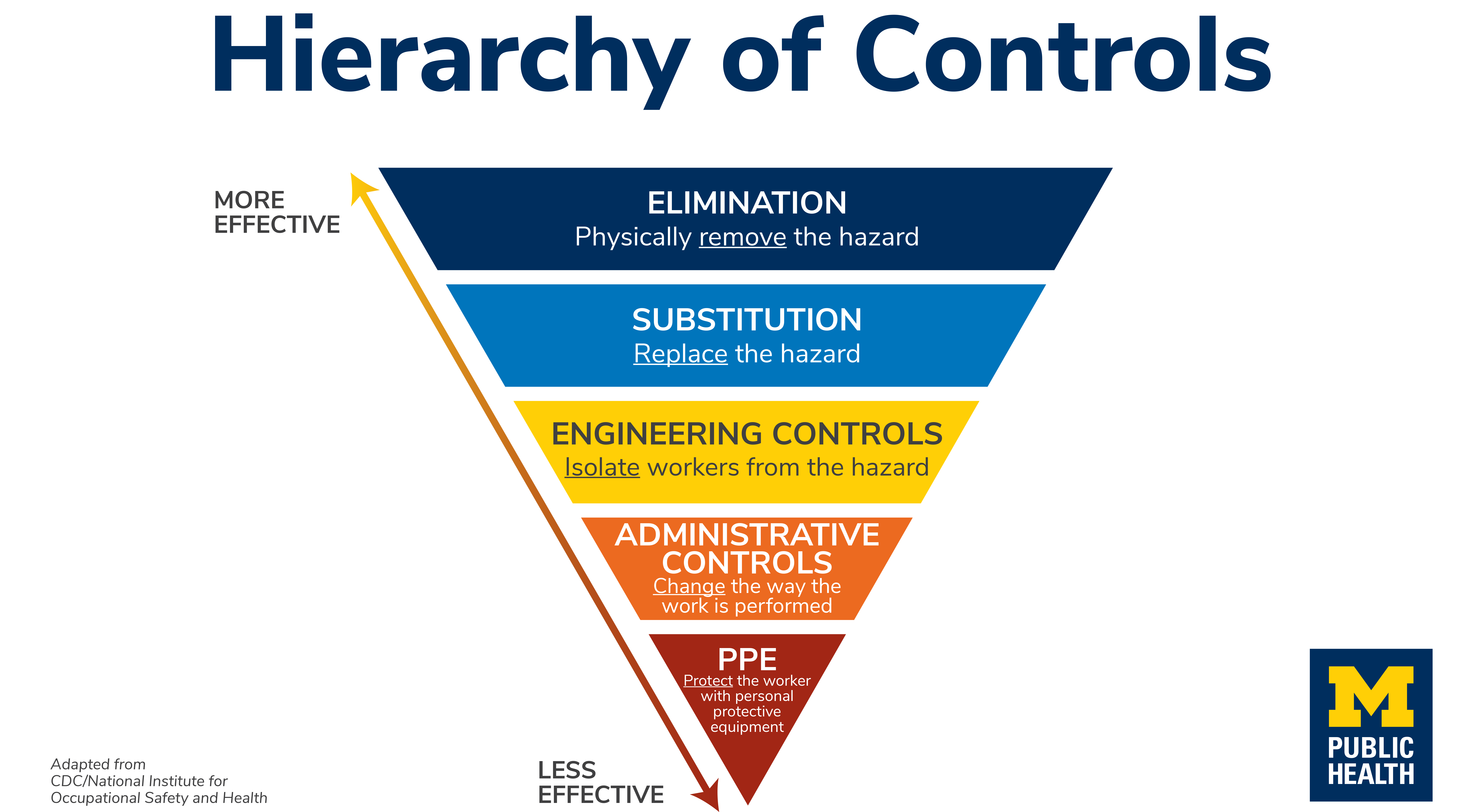
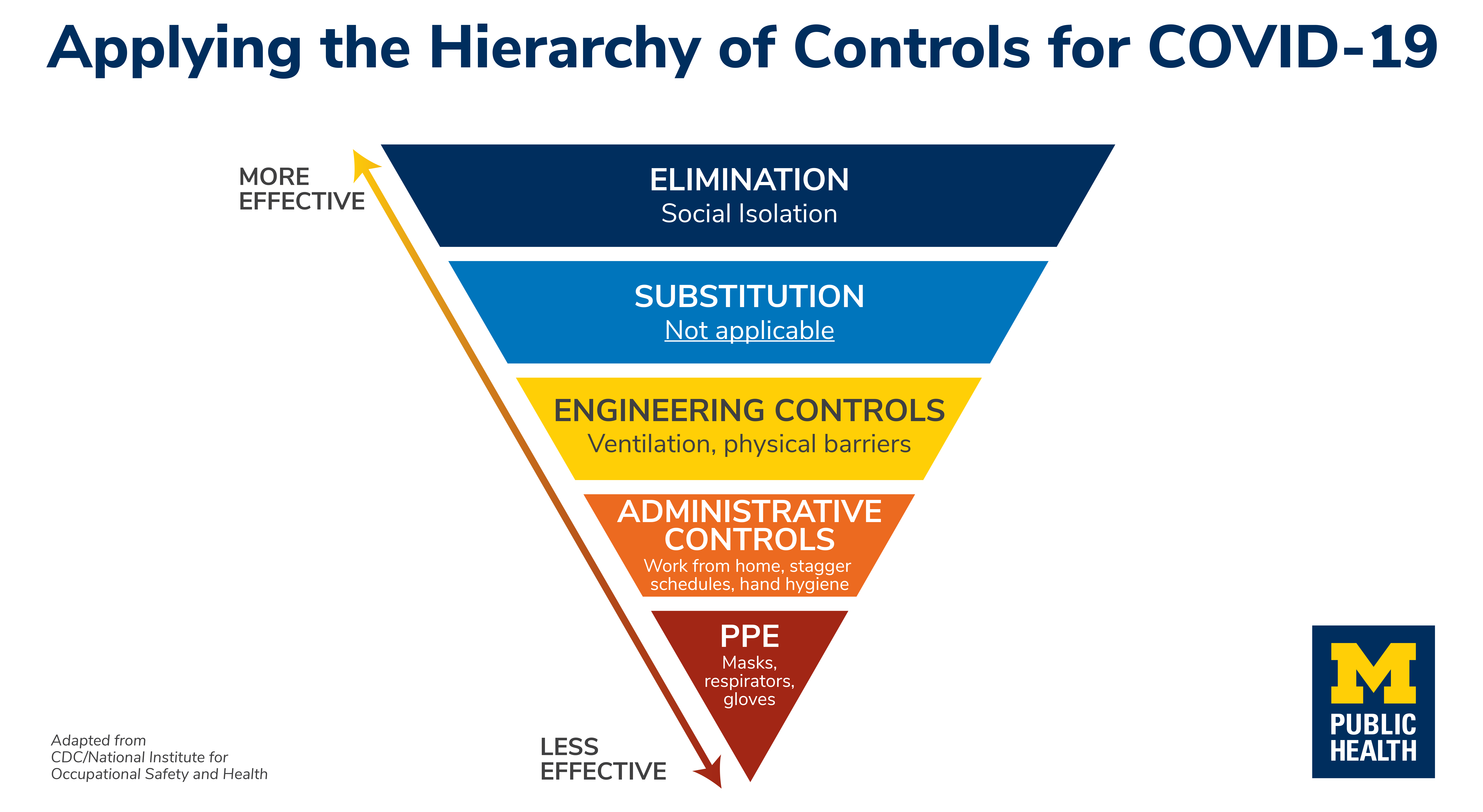
Restaurants are considered a higher risk operation because of all the public interaction. To move themselves into the medium-risk category, they can work from the Hierarchy of Controls chart [graphic here], a standard occupational health tool that makes improving worker safety clear, feasible, and attainable in most settings.
- Elimination. Physically removing “hazards” in a food-service setting means eliminating close contact
between employees and between employees and customers. Some chairs and tables will
be removed or certain sections of the restaurant closed off so patrons can sit further
away from each other. Customers can order on their own device and swipe their own
credit cards. You might pick up food from a counter. Each shift will likely include
fewer servers, cooks, hosts, and managers.
Substitution. We might see individual menus substituted out for a large menu on the wall or one-time use menus replacing the traditional plastic laminated menu. - Engineering Controls. Improved ventilation is very important with this virus—reconfiguring or upgrading an HVAC system will provide more air exchanges per hour. Installing barriers and shields to protect workers and making other physical changes, like adjusting the layout of kitchen station placement, will help.
- Administrative Controls. Changing how work is done could include: shift rotation, staggered start times, signage for customers, policies for employee time off and sick leave, providing additional training and education to employees before reopening, marking distances on the floor to encouraging customer spacing while waiting, virtual check-ins with customers waiting in the car until a table is open.
- Personal protective equipment (PPE). Restaurants should require all employees to wear some kind of facial covering, whether a mask or a shield. Those involved in food preparation should wear gloves and a face covering. Disposable PPE should be changed out regularly and non-disposal PPE should be disinfected regularly.
Each location will have specific challenges and opportunities, so owners and managers have to figure out what will work and what is realistic for their employees and their budget. In a perfect world, every workplace would have HEPA (high efficiency particulate air) filtration, a designation for any air filter that meets certain standards for extreme filtration of even the tiniest particles suspended in air.
Many workplaces do not have the financial means for that nor the infrastructure even to have their current HVAC system changed or retrofitted. Businesses and companies looking for support and evidence-based information should consult government health agencies like the Centers for Disease Control and Prevention (CDC) for information about disease control. For industry-specific information and support, they can look to their own industry’s national organization. The National Funeral Directors Association, for example, has great online resources for operating as safely as possible. Many others do too.
If you cannot find information for your industry, ask those at the top level of an organization or business, who should be working with safety professionals and/or industrial hygienists to develop new guidelines, policies, and practices to keep you and your coworkers safe and healthy. The National Institute of Environmental Health Sciences provides grants to deliver training to nonprofits so they can keep their workers safe.
What can a medium-risk location do to move itself to the low-risk category?
An example of a medium-risk group is a construction team, where they are working together and sharing tools but are mostly outside and do not engage the public much. Teams like this can determine a plan for sanitation—maybe one team member is designated to track shared equipment use and ensure it is sanitized regularly. Or everyone on the team could be responsible for sanitizing any tool they use once they finish using it.
In outdoor construction, social distancing is not as much of an issue. However, we still encourage measures like commuting alone rather than carpooling and taking breaks alone. The biggest obstacle in some of these settings is having an adequate number of hand washing stations or facilities. Portable sinks like what you see at fairs or outdoor festivals are encouraged so workers can clean their hands regularly without soap and water rather than relying solely on hand sanitizer.
- Interested in public health? Learn more today.
- Watch Michigan Public Health’s video about Returning to Work Safely.
- Read more articles about Environmental Health Sciences research at Michigan.
- Support research at Michigan Public Health.