COVID-19, Aerosols, and Ventilation

Q&A with Aurora Le
Assistant Professor of Environmental Health Sciences
According to the Centers for Disease Control and Prevention (CDC) and many other public
health experts, close contact with another person, and specifically through the spread
of respiratory droplets is considered the primary cause of infection from COVID-19.
However,mounting evidence points to aerosolized droplets—much smaller droplets that
remain in the air, sometimes for hours—as a concerning source of transmission for
coronavirus, especially in what are known as superspreader events, where many people
are infected by just a few or even one known source. 
As the weather gets colder and we find ourselves inside for longer periods of time, how can we avoid aerosolized droplets becoming a problem for disease transmission in our public buildings? We have many layers to consider for minimizing risk, but in many ways it starts with the ventilation systems in these buildings. To learn more about the connection between air ventilation and the COVID-19 pandemic, we spoke with Aurora Le, assistant professor of Environmental Health Sciences at the School of Public Health and an expert on biocontainment and biosafety procedures.
Why are we talking so much about ventilation and air circulation with the COVID-19 pandemic?
We know that COVID-19, like many other respiratory diseases, is spread primarily through droplet nuclei, which depending on the size of the droplets the larger ones will fall and settle within a few feet of a source due to gravity, whereas the smaller droplets can remain suspended in the air and potentially travel longer distances.
Air ventilation or air circulation refers to the distribution of fresh air into a room or other indoor space. Industrial hygienists and others who work in occupational safety and health more often use the term “ventilation.”
Air exchange rates or “air changes per hour” refers to the measure of air volume added or removed from a space in one hour divided by the volume of the space. Specifically in the case of COVID-19, aerosol transmission remains possible under the right conditions. Some examples are:
- A source generating a high enough infectious dose—a person sneezing, coughing, talking, singing, or spitting
- Nothing arresting or blocking that source—a mask or other facial covering, plexiglass shields or other physical barriers
- Environmental conditions that are conducive to viral survival (low temperature and humidity), low air exchanges per hour in a space
In assessing the ventilation of a space for infectious disease control, what are the basic factors we should consider?
Assessing your HVAC equipment for disease mitigation can be very complicated, but of course, it’s also important and worth going through the process. I generally would not recommend anyone trying to assess an HVAC system themselves; please refer to a trained industrial hygienist or trained ventilation specialist, as they likely can not only provide setup support but can run tests to ensure that your system is working properly.
It’s important to focus not on square footage of a room or other space but the overall volume. Higher ceilings increase the overall volume of a space; smaller spaces have less volume to diffuse germs and circulate air. Then you want to understand your air handling equipment. What type of HVAC system do you have, what’s its capacity, just how does it work and function properly? Some are single-zone systems and some are multi-zone. Some have a constant-volume supply of air and others have a variable-volume system. You’ll want to know if your system uses heat pumps, as that will affect airflow and humidity issues. Your manufacturer’s data and floor plans can provide a beginning blueprint for answering these questions. When you’re operating a big system like this, you also want to take into account practical things like your budget and your staff training to operate it properly. Fuel, electricity, and maintenance costs can be significant with HVAC systems. The proper timing of HVAC maintenance, filter replacements, and just installing a filter properly, is really important. You don’t want your system to be cost prohibitive, but you also want to supply your building with fresh, healthy air.
How often should air be fully circulated, or replaced, in each space?
Once you have a sense of the dimensions of your space and the capabilities of your HVAC systems to circulate air, you can focus on your airflow, how often air is being completely replaced in each space. Different spaces do have different recommendations depending on the type of room, and these are general, not specific to COVID. For example according to the American Society of Heating, Refrigerating and Air-Conditioning Engineers (ASHRAE), bedrooms should have 5-6 air exchanges per hour, kitchens 7-8; laundry rooms 8-9. These are about the size of room compared to the potential air quality hazards being produced in that space. But in general, most professionals in the industrial hygiene field suggest an air flow that gets you at least six complete air exchanges per hour, with three being a bare minimum for SARS-CoV-2. You want to understand the full picture of your air circulation from vents to cold-air returns, to make sure you don’t have blockages in the ductwork nor outside in the spaces, like furniture or plants or other object places in front of vents or returns. Airflow through vents and returns can be tested by professionals, and ductwork can be cleaned. Additionally, you want to know if you have natural ventilation in your space, like doors and windows that are frequently open, and if you have air movement created by special equipment like hoods in labs or kitchens or downdraft tables. In general, the goal is to ensure your HVAC system is aligned properly with your space.
How do temperature and humidity affect ventilation and disease mitigation?
Temperature and humidity must be taken into account, and your local climate will influence your ability to adjust humidity in your building. Here, it is important to understand the relationship between respiratory infectious diseases and humidity. Cold temperatures and low humidity create conditions in which certain viruses can stay viable in the environment for longer periods of time. That is to say, generally speaking, coronaviruses survive better in colder, dryer environments with low levels of ultraviolet light. When air is humid, aerosols become larger and therefore heavier. They fall out of the air and hit surfaces more quickly rather than staying in the air suspended for longer periods of time. As you look to maintain humidity in the winter months, you have to balance occupant comfort and aerosol reduction with mold growth. A relative humidity of 40-60% is ideal. Once you exceed 60% relative humidity, you increase the likelihood of mold growth, which has its own negative impacts on human health. You can purchase a quality hygrometer at a hardware store or online for well under $20 and adjust your HVAC system accordingly. If your system doesn’t include humidification options, then you’ll want to have some separate humidifiers operating in the winter.
How does human activity affect ventilation—from the activities that take place in each space to new problems that users can introduce?
First, you want to consider how your system is mixing fresh air coming from the outside with air that’s getting recirculated from the inside. Outside air might be fresher but also needs to be conditioned for temperature and humidity, which will add expense to your operations. Generally speaking, most buildings with central air conditioning are recirculating air from inside rather than drawing in fresh outside air. Again, look around at specific locations in the building where local exhaust vents in labs or kitchens might be drawing in outside air. With a system that uses air recirculation, you can safely filter the air to mitigate the presence of airborne pathogens like coronaviruses. It is essential that the people who manage the building know what type of ventilation system is in place, what kinds of filtration are being used, and how to ensure the system functions properly. Increasing air exchanges per hour does put an additional strain on the motor that is trying to move the air through your system, and you don’t want to diminish that optimal airflow through your building. So just be careful with decisions on air exchanges per hour, filtration and pay close attention to proper care and maintenance. Beyond that, we really can’t make blanket statements for all buildings related to temperature, humidity, and filtration. So make sure you take into consideration what is structurally there, how the building is being used, what your outdoor environment is like each season, and so on.
A good system that functions properly, even if it’s not brand new, can move air through your spaces effectively.
Second, human activity and building capacity are major considerations for ventilation needs. If you have a high volume of people doing physical activities—like exercising in a gym or singing and playing wind instruments in a music building—you are potentially increasing humidity and the force and volume with which people are expelling aerosolized droplets. Any high volume of human activity will increase the chances of the presence of infectious disease. New and recently remodeled buildings often require extra ventilation because new building materials off-gas manufacturing chemicals like formaldehyde at higher rates. Any building using large amounts of cleaning products regularly should implement extra ventilation regardless of the number of people present to maintain healthy air quality. Viral survival does go down over time, so if a space is unoccupied overnight, it gives you an opportunity to fully cycle your air without anyone present. You might reduce airflow at that point to reduce costs, but we do recommend leaving the ventilation system running at some level overnight.
Third, of course, is to pay close attention to user behavior. A great system designed to reduce exposure but not run properly won’t help as much as it could. If you don’t want windows or doors propped open, you should communicate those policies clearly to your building occupants. Maybe put stickers on windows and signs by doors. Is someone resetting the thermostats and fans to settings that are not ideal? Has someone placed a bookshelf or large plant in front of a vent or return? These are all part of the proper functioning of an HVAC system. We recommend running the exhaust fans in restrooms continuously so that individual users are not responsible for turning them on and off with the lights in those spaces.
I also want to stress that a good system that functions properly, even if it’s not brand new, can move air through your spaces effectively. You can spend a lot of money on new systems, new filters, and other equipment—and it can work really well. But if it’s not operated properly, it might be less effective than the system you replaced. A basic system running well is better than an expensive, complex system being run incorrectly.
Lastly and most importantly, air circulation, exchange, and filtration are just one part of what we call the Hierarchy of Controls, that graph you might have seen of stacked practices that work together to reduce disease transmission.
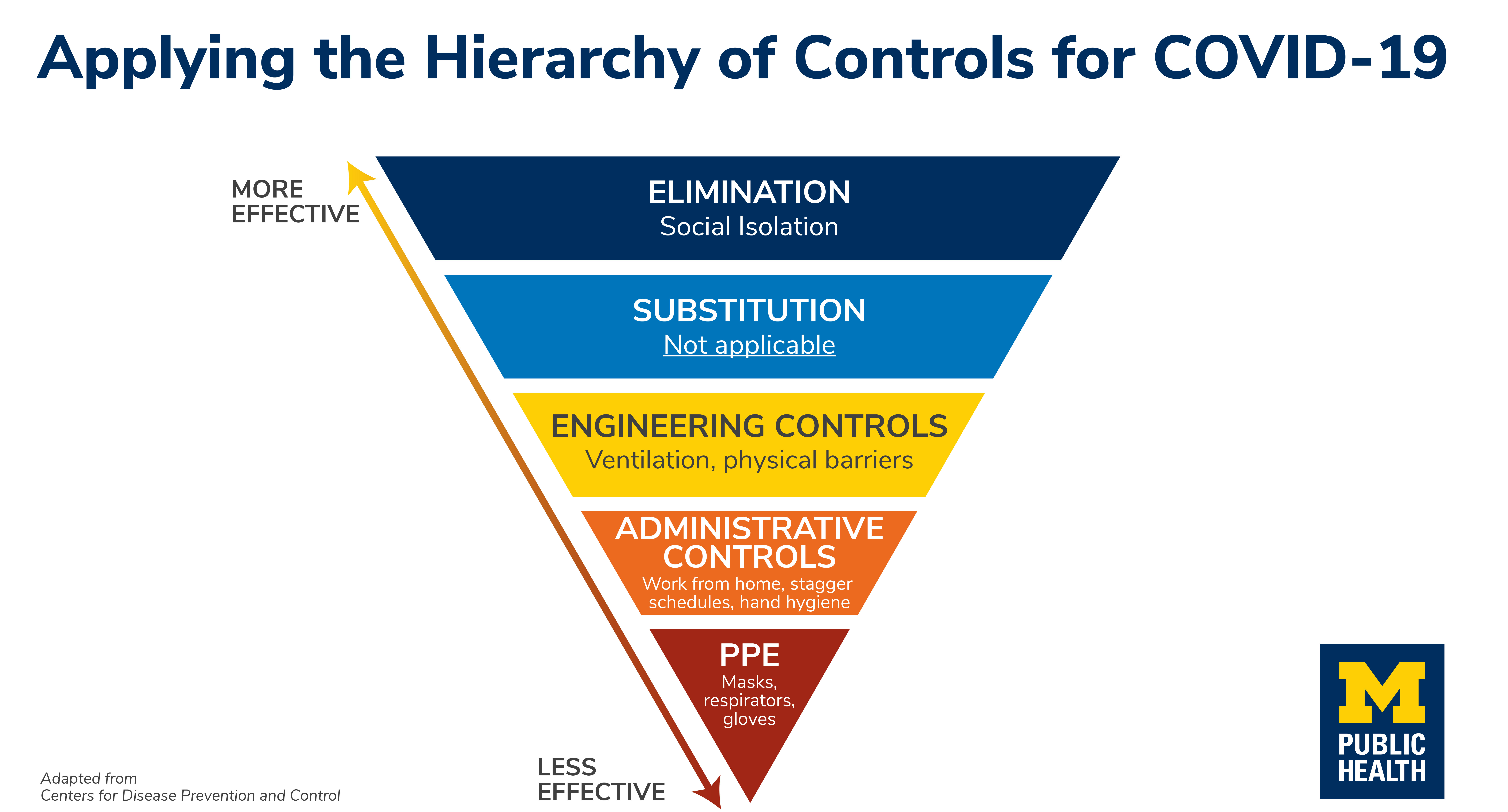
Ventilation is part of the engineering controls we can implement in a space to protect us from disease, along with plexiglass shields and other barriers. However you also have to keep an eye on public surveillance and how much COVID-19 is present in your community before you even consider entering a public space. When you do, you want to use a facial covering, like a mask, and you want to use administrative controls like social distancing and staggering who is in the building when. Air ventilation can help us reduce transmission of COVID-19, but it should not be considered the first line of defense (think about the Swiss cheese model of reducing respiratory infection risk).
In the field of biocontainment, we do not like to say that risks are eliminated. Rather, we say that risks can be minimized and reduced. So there is no such thing as an “entirely safe” space. Nevertheless you can do a lot with your building and with the behavior of the people in it to create safer environments for everyone there.
- Interested in public health? Learn more today.
- Watch Michigan Public Health’s video about Returning to Work Safely.
- Read more articles about Environmental Health Sciences research at Michigan.
- Support research at Michigan Public Health.
