Stacking Protections against Disease: What Do Driving a Car and Occupational Health Have to Do with the Coronavirus?

Aurora Le
Assistant Professor of Environmental Health Sciences
Preventing the spread of disease is essential for public health. So is having a steady income so we can support our basic daily needs, access health care, and maintain mental and social health.
So how can we go back to work safely and create economic security for Americans while we await a coronavirus vaccine?
Here’s where the public health fields of occupational health and industrial hygiene come in.
Stacking protective measures—using multiple layers of safeguards—is the only way to truly protect a worker.
Occupational health research tells us that stacking protective measures—using multiple layers of safeguards—is the only way to truly protect a worker from the potential harms of environmental exposures on the job.
Exposure to infection is one of those potential harms, and we regularly apply stacked best practices to control disease transmission in workplaces. In fact, as a biosafety and biocontainment expert focusing on facilities that work with highly infectious and dangerous diseases—including Ebola—I work on these approaches all the time.
What are stacked best practices?
A helpful way to think about stacked best practices is to think about all the things we do when we drive a vehicle safely.
If the entire population is safeguarded by successful, health-oriented infrastructures at the top, things like personal protective equipment at the bottom of the stack won’t be as necessary.
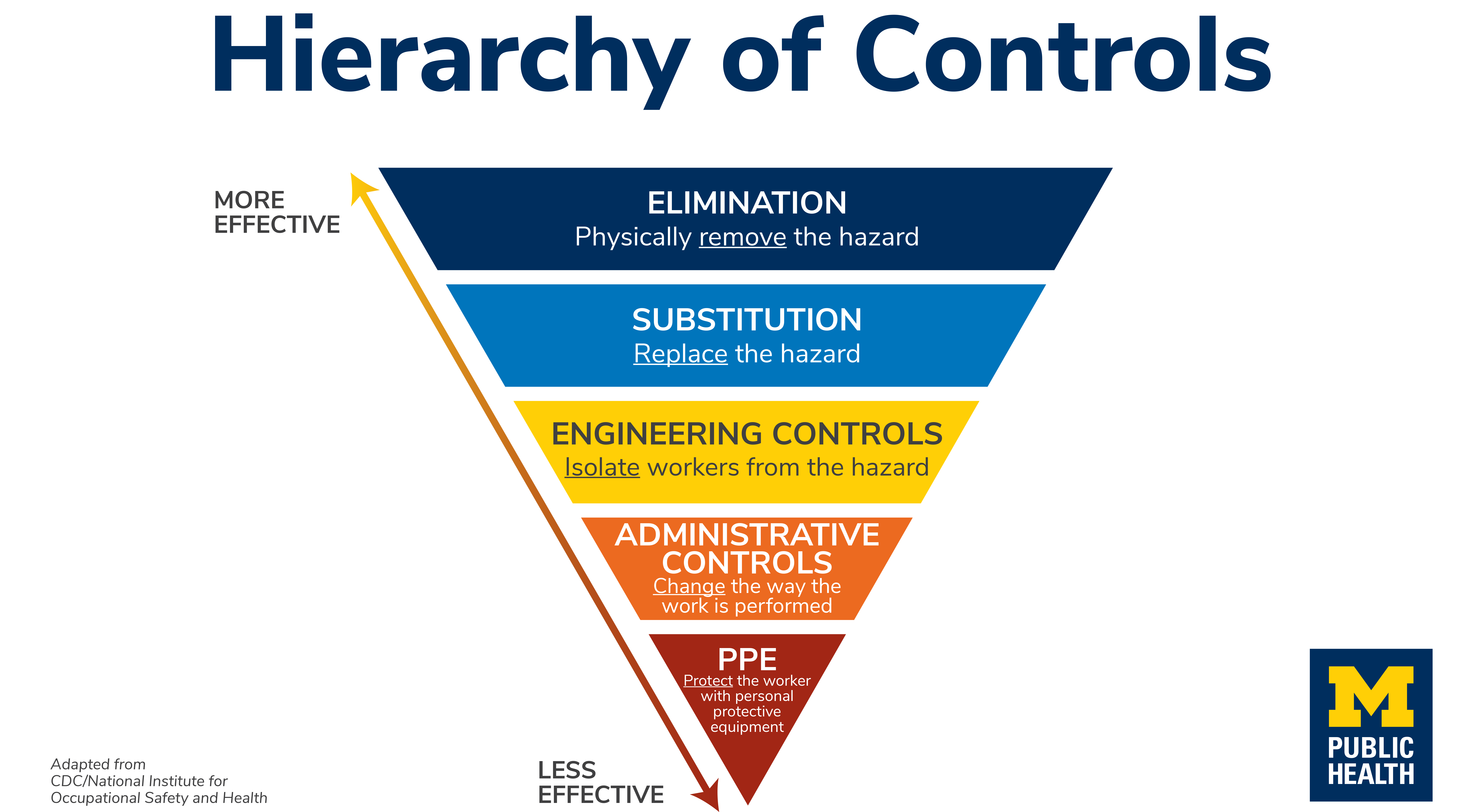
When we drive on a public road, we follow laws, regulations, and cultural norms that together give us a general sense of safety when everyone is doing their part. Occupational health experts tend to talk about these practices as moving from most effective down to least effective. If the entire population is safeguarded by successful, health-oriented infrastructures at the top, things like personal protective equipment at the bottom of the stack won’t be as necessary.
Public Health. Good public health infrastructure is often a victim of its own success. Public health has achieved a lot over the years—clean water, vaccinations, reduced lead contamination, and so on. But usually people think about public health only when things are going wrong.
Public health is focused on preventing disease and injury before it occurs, so we want to start off our driving situation by simply eliminating as many road risks as possible.
Public health is focused on preventing disease and injury before it occurs, so we want to start off our driving situation by simply eliminating as many road risks as possible. We build safe roads and repair cracks and potholes. We design safe cars and repair them when they don’t function well. If you drive under the influence, your license is revoked. We want to eliminate hazards before they have a chance to harm people.
We also must invest in our public health infrastructure. We can get better at surveillance, preparation, and response time to avoid the next pandemic before it starts. For now, to truly eliminate the risk of COVID-19, we will need a vaccine and herd immunity. This is a ways out, so we move down the stack.
Engineering. No matter how good our driving infrastructure, we will encounter risks, so we engineer our roadways and vehicles to make this activity more safe. We have traffic lights, stop signs and all kinds of other signs, lane markings, higher curbs in residential areas and guardrails on sharp curves. All of these things are engineered to make the roadways inherently as safe as possible for people.
Engineering controls in a workplace ensure a safe working experience, including protection from exposure to infectious disease.
Engineering controls in a workplace ensure a safe working experience, including protection from exposure to infectious disease—good water filtration systems, ventilation systems that exchange air more rapidly, physical barriers to prevent direct contact or at least the spread of respiratory droplets.
Administrative. We are all expected to follow certain rules of the road to maintain not only our safety but the safety of every other driver, every passenger, and anyone near a road who could become involved in a driving-related injury. Administrative controls are the things we do to change behaviors or to make behaviors safer—seatbelt laws, speed limits, expectations that people will not drive while intoxicated or texting. No one should be driving without a valid driver's license.
Administrative controls are the things we do to change behaviors or to make behaviors safer.
Administrative measures applied to infectious disease include things like social distancing recommendations, changing the way the workers and shifts are scheduled, adjusting overall schedules so that fewer people are on location on any given day. We also need to adjust our American attitudes about work culture, such as going in despite not feeling well. Moreover, we need to rethink our American policies about sick leave—many workplaces do not have adequate sick leave policies. People need to be able to stay home from work without fear of losing their job. Telecommuting and flex work hours should become more accepted. All of these things are designed to protect us from coming into contact with others who might be infected.
Personal. Personal protections on the road include wearing your seatbelt, making sure you are not driving under the influence, properly maintaining your vehicle to avoid accidents, using your turn signals and following the many other laws, rules, and guidelines for safe driving.
Some of the new things we’re all doing in light of the pandemic come from health care and other industries where biosafety is paramount.
Some of the new things we’re all doing in light of the pandemic come from health care and other industries where biosafety is paramount—wearing face coverings like masks and shields, wearing gloves, and replacing or disinfecting these items regularly. Basic personal hygiene like washing hands with soap and water, or at least using hand sanitizer, is extremely important. Disinfecting high-contact surfaces in your home and workplace is also helpful. Hopefully, using personal protective equipment (PPE) and practicing good personal hygiene will become accepted norms.
Why are stacked best practices so important?
Stacking these different levels of protection—public health interventions, engineering controls, administrative controls, and personal safeguards—gives us multiple layers of defense. If one level has flaws, the other layers include measures that will decrease the severity of that failure.
Stacking these different levels of protection gives us multiple layers of defense. If one level has flaws, the other layers include measures that will decrease the severity of that failure.
As this pandemic has progressed in the US, many workplaces have realized they have a lot more flexibility and resilience than they might have thought. Many organizations have proven themselves to be remarkably adaptable to this situation in a very short amount of time. That spirit of ingenuity and resilience will be a big part of our society overcoming this disease.
As we return to work with the need to drastically reduce our exposure to the coronavirus, each tactic you engage will give you more protection from disease and help reduce the spread of disease. The more layers we have, the less our risk of becoming infected.
About the Author
Aurora Le is assistant professor of Environmental Health Sciences at the University of Michigan School of Public Health. Le's research areas include highly infectious diseases and occupational safety and health. She works with the Biosafety and Infectious Disease Training Initiative (BIDTI) and supported the research efforts of the Nebraska Biocontainment Unit after the treatment of three Ebola patients there in 2014–2015.
- Interested in public health? Learn more today.
- Watch Michigan Public Health’s video about Returning to Work Safely.
- Read more articles about Environmental Health Sciences research at Michigan.
- Support research at Michigan Public Health.
